A person suffering from rectal prolapse has a part of the large intestine protruding from the anus. It happens because this part of the rectum has become abnormally stretched. This can be corrected by a rectal prolapse surgery where the rectum is placed in its proper location. The surgery can be done using different techniques. The surgeon will determine which would work best for your current health condition.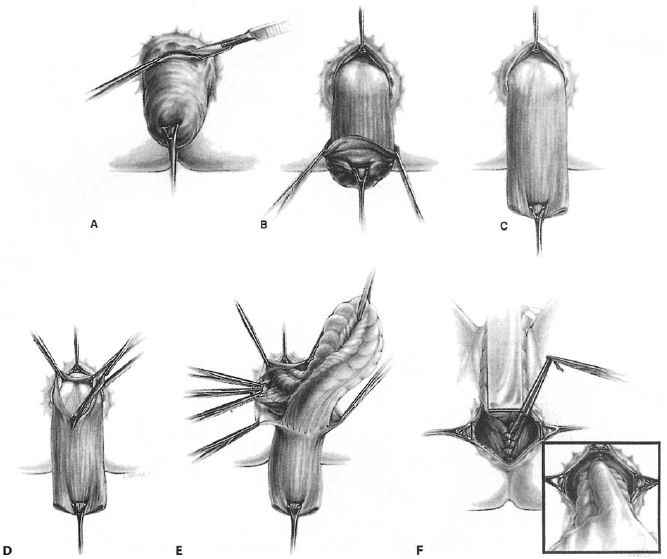
Do You Need a Rectal Prolapse Surgery?
People who have obstructed bowel movements, leaky stools, fetal incontinence or other chronic symptoms and are unable to push the rectum back will undergo a rectal prolapse surgery. A minor rectal prolapse can also occur when straining to pass your stool. If the prolapse happens occasionally, self-care measures are recommended and it usually goes away on its own.
Rectal prolapse is seen more often in elderly women. It can be prevented if a diet rich in fiber is consumed, along with lots of fluids. You can also take laxatives, stool bulking or softening agents.
What to Expect in a Rectal Prolapse Surgery
There are different ways of performing a rectal prolapse surgery. It can be either an abdominal open surgery with a large incision or through the perineum which is around the anus. The method depends on the causes of the prolapse, experience and preference of the surgeon as well as the health condition of the patient.
Abdominal Repair Approach
In abdominal repair approach, the rectum is pulled inside the body and attached to the tissues around the sacrum. This is done by either using a mesh which holds the rectum in place or with sutures. In a laparoscopic rectal prolapse surgery, several small incisions are made in the abdomen. A tiny camera and other surgical tools are inserted through these incisions to repair the rectal prolapse. General anesthesia is administered during the surgery.
Perineal Repair Approach
In perineal repair approach which is performed through the perineum, a local anesthesia is administered. It is usually done on elderly people who are not able to go through abdominal surgery. In Altemeier procedure for rectal prolapse, part of the rectum and sigmoid is removed and attached to the colon. In the Delorme procedure on shorter prolapse, only the lining of the rectum is removed and the shortened rectum is connected to the muscular layer.
Complications of Rectal Prolapse Surgery
1. Infection
One of the most common complications of rectal prolapse surgery is infection which is caused by the organisms present in the skin around the wound. Infection can also be caused by foreign implants. Infection after perineal procedure is rare, however, there can be perineal anastomosis.
2. Bleeding
Bleeding is seen if there is tearing of presacral veins or when the mesh and rectum is attached directly to the presacral fascia. To control the bleeding, the first measure is to apply pressure on the area for 10-15 minutes. If this does not help, tamponing the vessels is done by placing titanium thumbtacks.
3. Bowel Injury
When the rectum is mobilized, there can be chances of bowel injury which can be repaired when identified. No foreign material should be used in case of bowel injury. If the injury goes unrecognized, it can cause abscess or pelvic sepsis. Unrecognized bowel injuries can happen due to laparoscopic method.
4. Anastomotic Leakage
Any procedure that involves anastomosis has the risk of leakage. If the leak is small and contained, there is no requirement of re-exploration. Supportive care can resolve the problem. For large leaks, urgent re-exploration is required. If the anastomosis is completely disrupted, stapling or over-sewing the rectal stump should be done.
5. Change in Bladder and Sexual Function
If the abdominal rectal prolapse surgery is performed correctly, it can rarely cause changes in the bladder and sexual functioning. Since the pelvic sympathetic and parasympathetic nerves are present along the rectum, incorrect dissection can lead to impotence, retrograde ejaculation or bladder dysfunction.
6. Constipation
Outlet obstruction is not often caused by perineal procedure or anterior resection. It used to happen earlier when rectum was tacked to the sacrum circumferentially.
Care After Rectal Prolapse Surgery
Some of the general guidelines to follow at home after a rectal prolapse surgery are:
- Take as much rest as possible.
- Try to avoid lifting heavy objects.
- Do not strain while passing stools.
- Eat high fiber food and drink lots of water.
- If you have fever, heavy bleeding, difficulty in urinating, signs of infection around the wound site, contact the doctor.
- You can resume work about six weeks after surgery.
- Make sure you do not skip follow-up visits.
- If you have had rectocele surgery, it is normal to have bloody vaginal discharge for some time.
How Long Does It Take to Completely Recover?
The patients will be required to stay in the hospital for around three to five days on an average. However, the exact healing time depends on the patients’ health conditions. Normally, it will take around three months to completely recover. But the patients should still avoid lifting heavy objects and straining on the toilet for up to six months. To prevent any prolapse from recurring, patients should avoid any activities which put pressure on the abdomen for lifetime.